In a sunlit living room in suburban Boston, a 57 year old teacher named Margaret Ellis stared at the array of pill bottles that had failed to ease her persistent anxiety and spiritual disconnection. After two decades of standard therapy protocols that treated her symptoms as interchangeable with anyone elses, she enrolled in a program that examined her brain activity, sleep rhythms, genetic markers and daily digital footprint. The result was a care plan unlike anything she had encountered. This is the frontier of personalized mental health, where artificial intelligence, neuroscience and vast streams of personal data converge to shape treatments as unique as fingerprints. What was once science fiction is now entering clinical practice, offering millions of middle aged Americans a chance to address both emotional distress and deeper questions of meaning.
The Shift From Generic Treatments To Tailored Approaches

For generations mental health care relied on broad diagnostic categories and standardized interventions. A diagnosis of depression might lead to the same antidepressant and weekly talk therapy regardless of whether the patient was a stressed executive or a grieving retiree. That model is giving way to something more precise. Clinicians now integrate multiple data sources to understand the distinct biological and environmental factors shaping each persons experience. The change reflects growing recognition that mental suffering arises from countless unique pathways. What relieves one individual may do nothing for another. This evolution promises not only faster relief but also fewer wasted months spent on approaches that were never suited to the patient in the first place.
How Artificial Intelligence Analyzes Individual Patterns

Artificial intelligence has become central to this transformation. Machine learning algorithms can process speech patterns from therapy sessions, text from journaling apps and even subtle shifts in social media behavior to detect early signs of distress. These systems identify correlations invisible to the human eye. One platform developed at Stanford analyzes voice recordings for acoustic features linked to mood disorders with remarkable accuracy. When Margaret entered such a system her recorded conversations revealed patterns of rumination that her previous therapists had missed. The AI then suggested specific cognitive exercises timed to her daily energy cycles. Proponents argue this technology extends the reach of care by providing continuous insight between office visits.
Neuroscience Offers New Windows Into The Brain
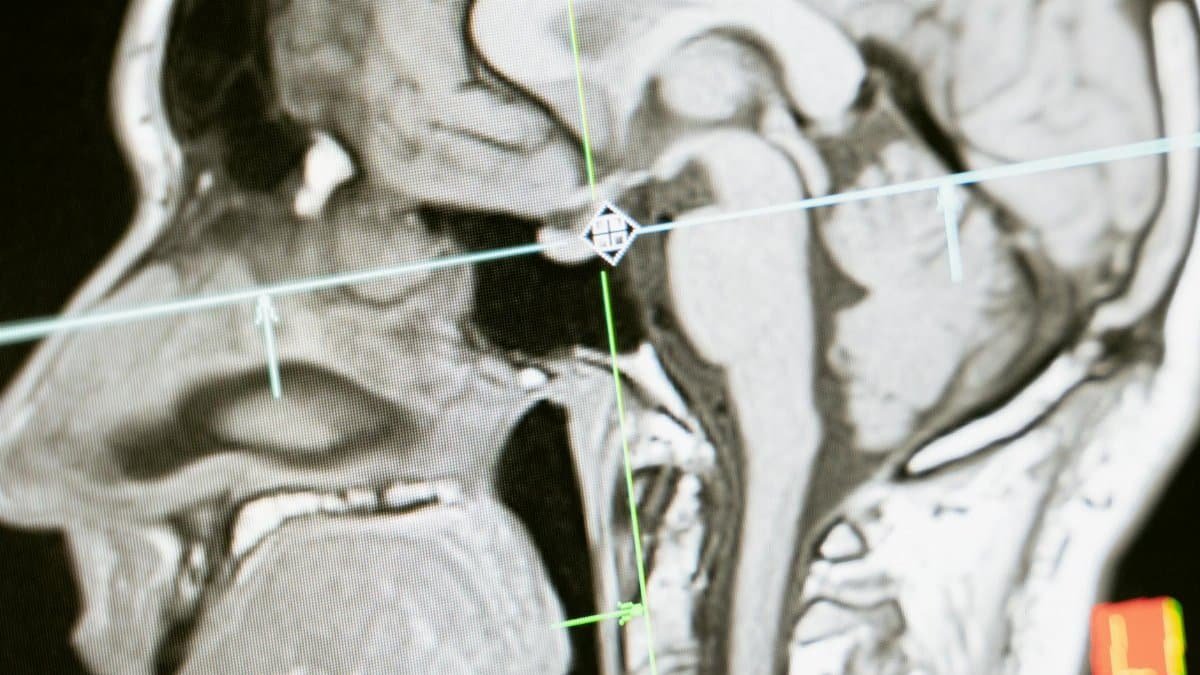
Advanced imaging techniques are revealing that no two brains respond to stress or sadness in exactly the same way. Functional magnetic resonance imaging can show which neural circuits are underactive in a particular patient allowing psychiatrists to select interventions that target those areas. Some clinics now use electroencephalogram readings to guide transcranial magnetic stimulation treatments customizing the frequency and location of pulses. These methods move mental health care closer to the precision long seen in oncology where tumor genetics dictate the chemotherapy regimen. The result is a form of brain informed treatment that respects the biological individuality of each person rather than forcing them into preexisting boxes.
The Growing Influence Of Big Data In Care Decisions

Information gathered from wearable sensors fitness trackers and even credit card purchases when properly consented is helping build comprehensive behavioral profiles. Heart rate variability sleep quality physical movement and location patterns all feed into predictive models that forecast potential crises before they fully develop. A pilot project in California used aggregated anonymized data to identify patients at risk of severe depression weeks in advance. Clinicians could then intervene with tailored support ranging from increased therapy sessions to recommendations for community volunteering that addressed both emotional and spiritual needs. This data driven layer adds an objective dimension to what has traditionally been a largely subjective field.
Connecting Technology To Spiritual Growth And Awareness

One of the most intriguing developments involves weaving spiritual dimensions into personalized mental health frameworks. Rather than treating spiritual questions as separate from clinical symptoms some programs now use neural feedback to recommend specific contemplative practices. For individuals whose brain scans show strong activity in areas associated with awe and transcendence the system might suggest nature immersion or guided meditation focused on compassion. Others receive prompts for reflective writing or participation in faith communities calibrated to their psychological profile. This integration recognizes that many middle aged adults seek not only symptom reduction but renewed sense of purpose and connection. Technology in this context becomes a bridge rather than a barrier to deeper existential exploration.
According to a recent report from the American Psychological Association facilities that combine neuroscientific data with patient reported spiritual values show higher rates of sustained recovery than those using either approach alone.
Genetic Testing Opens Doors To Precision Medicine

Pharmacogenomic testing has begun to change how medications are prescribed. Simple cheek swabs can reveal how an individuals body metabolizes different antidepressants reducing the trial and error period that often discourages patients. One woman in her early 60s avoided three medications that her genetics suggested would be ineffective or cause severe side effects. Instead her doctor selected a different compound that worked within weeks. While genetic data represents only one piece of the personalized mental health puzzle it adds crucial biological context that can prevent months of frustration and dangerous side effects.
Wearable Devices Provide Continuous Valuable Feedback

Consumer wearables have evolved from simple step counters to sophisticated mood laboratories. Devices tracking skin conductance heart rhythms and movement can now alert users and their care teams to rising anxiety levels in real time. Some systems automatically suggest brief breathing exercises or connect users with on call therapists when patterns indicate distress. For middle aged individuals juggling careers family responsibilities and aging parents these tools offer a safety net that fits into busy lives. The continuous stream of information also helps patients notice connections between their physical state and emotional well being that might otherwise remain hidden.
Patient Experiences Highlight The Benefits Of Customization
Margaret Ellis is not alone in her positive outcome. Across the country individuals report that personalized plans help them feel truly seen for the first time. A 48 year old software engineer whose depression resisted conventional treatment discovered through brain mapping that his symptoms were closely tied to irregular circadian rhythms. Adjusting his schedule and adding carefully timed light therapy produced results that years of medication had not. Stories like these are becoming more common as clinics adopt multimodal assessment techniques. Patients often describe the experience as liberating describing a shift from passive recipient of care to active participant in a collaborative process.
Navigating Ethical Questions And Data Protection

This rush toward personalization brings serious responsibilities. Who owns the intimate data collected from brains and daily habits? How can vulnerable patients be protected from misuse of predictive algorithms by insurance companies or employers? These questions loom large as the field expands. Privacy advocates urge strong regulations and transparent consent processes. Equally important is ensuring that algorithmic recommendations do not reinforce existing biases in mental health research which has historically focused on certain demographic groups. Responsible implementation will require ongoing dialogue between technologists clinicians ethicists and the people whose lives are being mapped.
Barriers To Widespread Adoption And Possible Solutions

Despite the promise cost and access remain significant obstacles. Comprehensive brain imaging and genetic testing are expensive and often not covered by insurance. Rural communities and lower income households risk being left behind in what could become a two tiered system of mental health care. Some innovators are working on more affordable alternatives such as smartphone based voice analysis and virtual reality assessments that require less specialized equipment. Telehealth platforms are also expanding access to practitioners trained in these integrated methods. Public policy will need to evolve quickly if the benefits of personalized mental health are to reach beyond affluent early adopters.
What The Future May Hold For Integrated Care

Looking ahead the convergence of artificial intelligence neuroscience and personal data seems likely to accelerate. Within the next decade some experts envision systems that seamlessly blend clinical metrics with an individuals values spiritual orientation and life goals. Treatment plans might incorporate everything from medication and therapy to specially designed contemplative apps or community service recommendations. The goal is not simply the absence of symptoms but the presence of vitality purpose and resilience. For millions of middle aged Americans who have quietly wondered whether lasting change was possible these developments offer something rare in mental health care: genuine reason for optimism grounded in science yet respectful of the full complexity of human experience.
By Natasha Weber
