In the heart of Boston dedicated nurses have reached a critical juncture in their relationship with hospital administration. At Tufts Medical Center a vote of no confidence has highlighted deep seated issues with staffing in the operating rooms. These Tufts nurses concerns have brought to light serious questions about patient safety and the ability of staff to perform their duties effectively. The situation has captured the attention of the community as it touches on fundamental aspects of trust in the institutions responsible for our health. As middle aged Americans who may one day rely on such facilities many readers will find this story particularly relevant to their own lives and the welfare of their loved ones. The conflict points to a larger struggle within American healthcare where the ideals of compassionate care collide with the realities of budget constraints and workforce challenges.
A Historic Vote Of No Confidence

The nurses at Tufts Medical Center took an extraordinary step when they overwhelmingly supported a declaration of no confidence in top administrators. Union tallies showed support exceeding eighty five percent among those who participated. This was no impulsive gesture. It followed more than a year of internal appeals and documented reports about unsafe conditions in surgical settings. The Boston Globe has chronicled how these efforts gained momentum after several near misses in the operating rooms where delays in response times raised alarms. Nurses described arriving for shifts only to discover they would manage multiple complex cases with minimal backup. Such conditions they argue erode the very foundation of quality care. The vote has now placed public pressure on the institution to respond with more than promises.
Daily Struggles In The Operating Suite
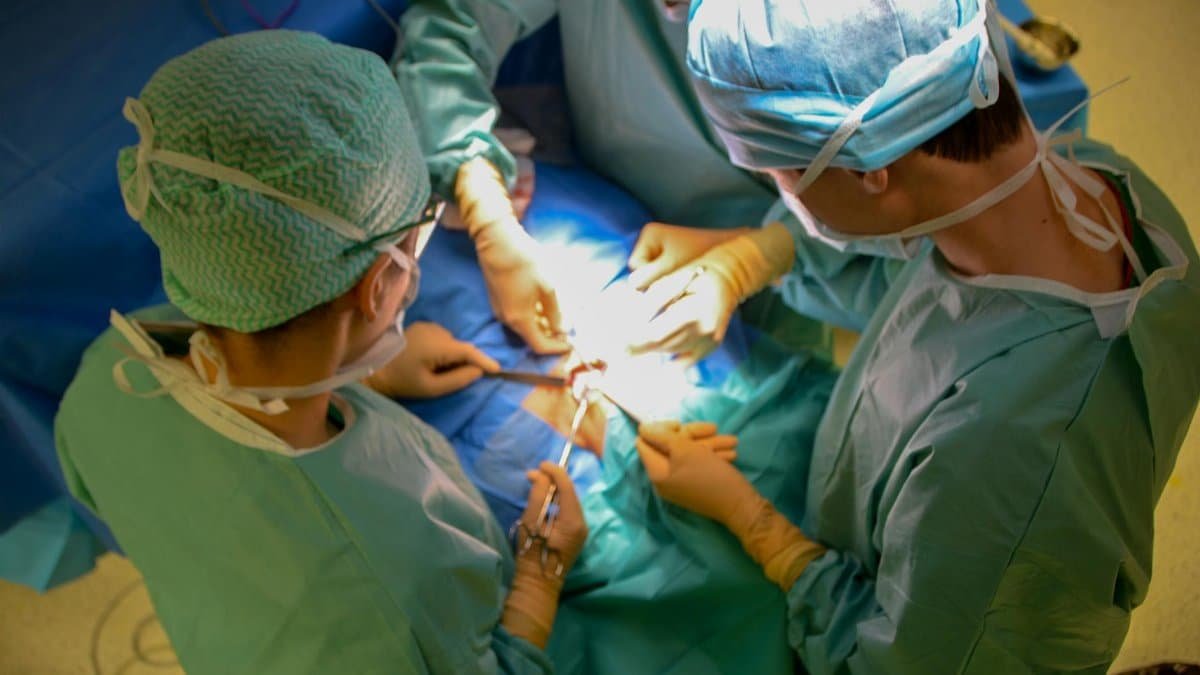
Inside the surgical department at Tufts Medical Center the pace is unrelenting. A typical shift demands coordination among scrub technicians circulating nurses and specialized anesthesiologists. When staffing falls short one nurse may find herself responsible for tasks that normally require three sets of hands. Equipment must be prepared monitors adjusted and sterile fields maintained without interruption. Fatigue sets in quickly under these demands. Many nurses report working twelve hour stretches with barely enough time to hydrate or review critical patient histories. These patterns have become commonplace according to staff interviews. The result is a workplace where vigilance the cornerstone of surgical success sometimes wavers not because of individual shortcomings but because the system asks too much of too few.
Risks To Patients From Inadequate Staffing

Patient safety emerges as the central issue in discussions around Tufts nurses concerns. Medical studies have long established clear links between staffing levels and surgical outcomes. When teams are stretched errors in counting instruments miscommunication during handoffs and delayed recognition of complications become more likely. One analysis from the Massachusetts Nurses Association shared at public forums cited data suggesting that understaffed operating rooms experience complication rates up to twenty five percent higher than fully supported ones. At Tufts Medical Center nurses have recounted incidents in which emergency responses were slowed because available personnel were already committed to other procedures. For patients facing everything from routine gallbladder removals to delicate cardiac repairs these delays carry real consequences. Families expect excellence when they entrust loved ones to the operating table. Persistent shortages challenge that expectation.
Leaderships Perspective On The Crisis

Hospital administrators acknowledge the pressures while pointing to broader industry obstacles. In statements released after the vote Tufts Medical Center officials noted the national shortage of trained operating room nurses as a primary driver. They highlight recent investments in training programs and competitive hiring bonuses aimed at expanding the workforce. Recruitment remains difficult they explain because younger professionals often seek different lifestyles than the demanding schedules of surgical nursing require. Officials also cite financial realities facing academic medical centers that balance cutting edge research with clinical care. While they express commitment to addressing feedback they stop short of promising immediate increases in staffing ratios. This measured response has done little to reassure those working on the front lines who seek faster action.
Voices From The Nursing Staff

Many nurses have chosen to speak through their union rather than individually fearing repercussions. Those willing to share stories paint a consistent picture of dedication mixed with disillusionment. One veteran with more than twenty years at the center described the joy of helping patients heal only to see that satisfaction overshadowed by constant worry about what might be missed. Another recalled canceling long planned family vacations after being called in repeatedly to cover shortages. These accounts reveal a workforce that still feels called to the profession yet increasingly doubts whether the institution values their expertise. Their collective message is simple: respect for their professional judgment must translate into adequate support during the most intense moments of patient care.
The Spiritual Toll On Healthcare Workers

Beyond the measurable statistics lies a deeper cost that touches the spirit of nursing itself. Many view their work as a form of service rooted in compassion and presence. When chronic understaffing prevents them from offering that full presence moral injury follows. Nurses describe leaving shifts haunted by the sense that they have not been able to advocate fully for their patients. This erosion of purpose can lead to emotional exhaustion that travels home with them affecting relationships and personal health. In an era when many middle aged Americans seek greater meaning in their own vocations the experiences reported at Tufts Medical Center resonate. If even those called to heal find their spirit diminished by systemic failures then society must ask what values truly guide our healthcare institutions. Restoring the sense of sacred duty in nursing may require more than better pay. It demands environments where caregivers can practice with integrity.
National Context Of Labor Shortages In Medicine

The situation at Tufts Medical Center mirrors challenges seen across the country. From rural community hospitals to major urban centers staffing shortages in surgical departments have grown more acute since the pandemic. An aging population requires more procedures while many experienced nurses have retired or shifted to less stressful roles. Travel nursing has become a temporary fix yet it brings its own disruptions to team cohesion. Professional organizations report that nearly one in five nursing positions nationwide remain unfilled. This context does not excuse local shortcomings but it does explain why Tufts nurses concerns reflect a national pattern rather than an isolated failure. Policymakers continue to debate solutions including expanded training pipelines loan forgiveness for nursing graduates and regulatory reforms around safe staffing ratios.
Potential Solutions To Ease The Pressure

Creative approaches could help address the core issues. Some hospitals have successfully implemented tiered staffing models that pair experienced nurses with carefully trained support staff for appropriate tasks. Others have embraced technology such as advanced monitoring systems that free personnel from constant manual observation. At Tufts Medical Center nurses have proposed formalized ratios specific to operating room complexity rather than generic formulas. Union leaders suggest joint committees where frontline staff and administrators share decision making around scheduling and hiring. Investment in mentorship programs might also encourage newer nurses to specialize in surgical care by offering them guidance and career pathways. Whatever combination is chosen success will depend on genuine collaboration rather than top down mandates.
Union Efforts To Amplify These Issues

The Massachusetts Nurses Association has played a key role in elevating Tufts nurses concerns to public attention. Through press conferences and community outreach the union has framed the dispute as part of a larger fight for both worker dignity and patient protection. They have called for state level hearings to examine staffing practices at academic medical centers. Their advocacy includes legal review of whether current conditions violate existing labor agreements or safety regulations. By connecting local experiences to statewide trends the union aims to build momentum for systemic reform. Not everyone agrees with their tactics. Some observers worry that public votes of no confidence may damage the hospitals reputation in ways that ultimately harm recruitment. Still the union maintains that silence would only perpetuate unsafe conditions.
Looking Ahead For Quality Care In Boston

The coming months will prove decisive for Tufts Medical Center and its dedicated nursing staff. If administrators and caregivers can find common ground the episode might become a catalyst for stronger teams and safer protocols. Failure to resolve the underlying tensions could accelerate departures of skilled professionals at a time when Boston needs them most. For readers who value reliable healthcare the story serves as a reminder that quality depends on more than shiny facilities and advanced equipment. It rests on the well supported professionals who show up ready to care. The Tufts nurses concerns have made clear that when that support falters everyone ultimately pays a price. Restoring balance will require honest dialogue sustained investment and a renewed commitment to the human element at the heart of medicine. Bostonians watching this unfold hope the resolution honors the profound responsibility healthcare workers carry each day.
(Word count: 1,287)
