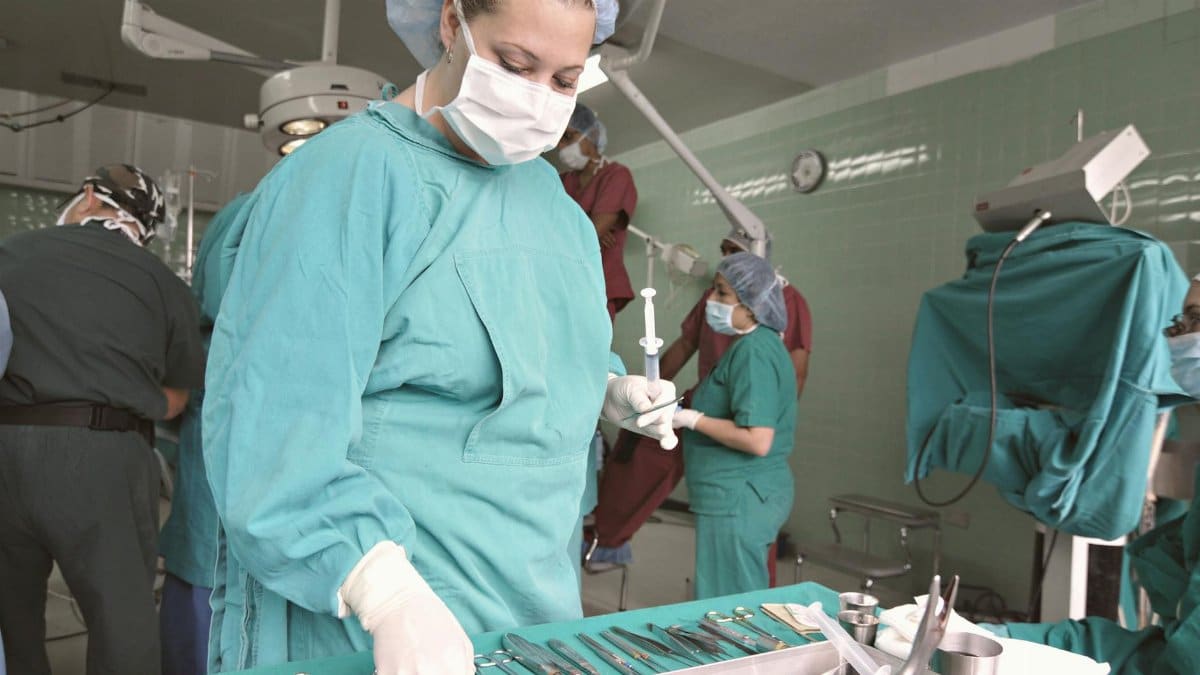
In the bustling corridors of Tufts Medical Center a profound unease has settled among those who provide care during the most critical moments. Nurses assigned to the operating rooms have grown increasingly vocal about conditions that they believe compromise both their ability to perform effectively and the safety of the patients who entrust them with their lives. Recently these professionals took the significant step of holding a vote of no confidence in the hospital administration. This development has cast a spotlight on what many describe as chronic understaffing in areas where precision and focus are paramount. The Tufts nurses concerns revolve around having too few experienced hands available during complex procedures. Such shortages they argue lead to fatigue and heightened potential for error in environments where mistakes can have lasting consequences. As the debate intensifies it raises questions about priorities in healthcare delivery today and what it means to truly care for others in their most vulnerable states.
The Mounting Pressures in Operating Rooms
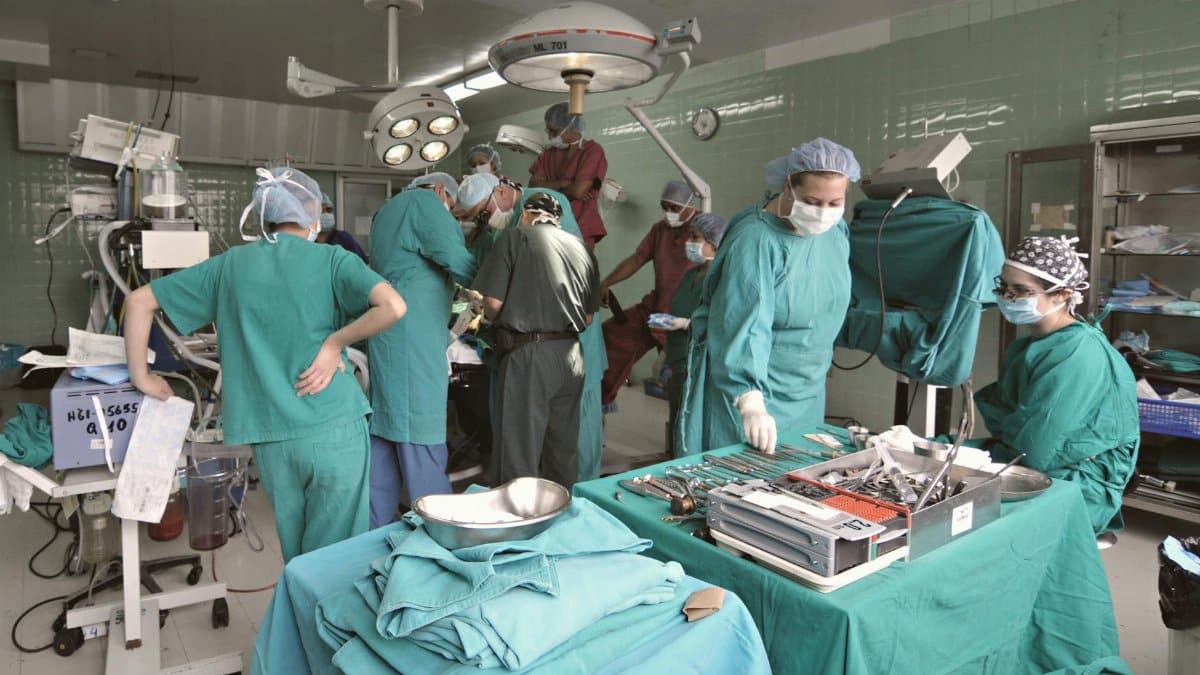
Operating rooms demand absolute concentration yet the reality at Tufts Medical Center often falls short of that ideal. Nurses report being stretched across multiple cases with insufficient support staff to monitor vital signs prepare instruments or respond to unexpected complications. One circulating nurse might find herself responsible for three simultaneous procedures a situation that would have been unthinkable a decade ago. These pressures have built over several years as the hospital has faced challenges in recruitment and retention. The physical layout of the surgical suites adds another layer of difficulty with staff needing to cover large distances quickly while carrying heavy sterile trays. Many seasoned nurses say the pace has become unsustainable and it affects their ability to deliver the level of attention that patients deserve. This environment has transformed what should be a place of healing into one of constant tension.
Understanding the Vote of No Confidence

The vote of no confidence represents more than simple dissatisfaction. It signals a complete breakdown in trust between frontline caregivers and those who set policy. More than eighty percent of eligible nurses participated in the recent ballot with an overwhelming majority expressing deep reservations about current leadership decisions. Such votes remain rare in healthcare settings because they carry significant professional risk for those involved. At Tufts this action came after months of documented complaints through official channels that produced little visible change. The nurses association has emphasized that this was not a hasty decision but rather the culmination of years of eroded conditions. By taking this public stand the staff hopes to force meaningful dialogue rather than continued promises that fail to materialize in actual staffing improvements.
Examining Specific Staffing Issues

Current ratios in the operating rooms frequently violate recommended standards established by professional organizations. Where guidelines suggest one dedicated nurse per patient during critical phases the hospital has at times operated with ratios twice as high. Specialized roles such as scrub nurses and anesthesia support have seen particularly acute shortages. Experienced personnel who once formed the backbone of the team have left for facilities offering better compensation or more reasonable schedules. New graduates arrive but often lack the advanced training necessary for complex cases involving cardiac or neurological procedures. This creates a dangerous knowledge gap that cannot be bridged overnight. Internal records obtained by reporters show repeated instances where surgeries were delayed or rescheduled due to inadequate personnel rather than medical necessity.
Patient Safety Emerges as Central Issue

Patient safety stands at the heart of the Tufts nurses concerns. When staffing falls below safe levels the risk of preventable errors rises sharply. Studies from major research institutions have consistently demonstrated this connection. A comprehensive review published by the Agency for Healthcare Research and Quality found that inadequate nurse staffing correlates with increased rates of surgical site infections wrong site procedures and postoperative complications. The link can be found here: https://www.ahrq.gov/patient-safety/index.html. At Tufts nurses describe situations where they simply cannot maintain the constant vigilance required to catch subtle changes in patient status. Near misses have become more common according to internal incident reports though the hospital maintains that overall safety metrics remain within acceptable parameters. The nurses counter that those metrics fail to capture the full picture of what occurs inside individual operating rooms.
Hospital Leaders Offer Their Perspective

Administrators at Tufts Medical Center acknowledge the challenges while pointing to efforts already underway to address them. In statements released following the vote officials noted that they have hired more than twenty new surgical nurses in the past eighteen months and continue aggressive recruitment campaigns. They cite the national nursing shortage as a primary factor beyond any single institution control. Hospital representatives emphasize their commitment to competitive salaries and improved benefits packages designed to attract and retain talent. They also highlight recent investments in training programs intended to prepare newer staff for the demands of operating room work. While expressing respect for the dedication of their nursing staff leadership maintains that dramatic changes cannot occur instantly and that progress is being made even if it feels too slow for those on the front lines.
National Trends Affecting Local Hospitals

The situation at Tufts reflects broader patterns visible across the United States. Hospitals in every region report similar difficulties attracting and keeping experienced surgical nurses. An aging workforce combined with burnout accelerated by recent public health crises has created a structural imbalance. Massachusetts has fared somewhat better than some states yet urban medical centers like Tufts still struggle against the pull of suburban facilities offering less intense workloads. Economic pressures have forced many institutions to operate with leaner staffs in pursuit of financial sustainability. These national trends provide important context for understanding why the Tufts nurses concerns have proven so difficult to resolve. Without coordinated action at state and federal levels individual hospitals may find themselves locked in perpetual competition for the same limited pool of qualified professionals.
Nurses Share Their Experiences

Those working directly with patients offer the most compelling accounts of daily reality. One nurse with fifteen years at Tufts described arriving for a shift only to learn she would be covering two complex orthopedic cases simultaneously with limited assistance. Another recalled a situation where a patient experienced sudden bleeding during surgery and the delayed response time stemmed directly from insufficient available hands. These stories emerge not as isolated incidents but as representative examples of systemic strain. Many nurses speak of the emotional toll that comes from knowing they cannot provide the care they believe patients deserve. The pride they once took in their specialized skills has been replaced by persistent anxiety about potential oversights. Several have chosen to speak publicly despite fearing repercussions because they feel the issue has reached a breaking point.
Exploring the Moral Dimensions of Care

Beyond the statistics and schedules lies a deeper ethical question that touches on the very vocation of nursing. Many who enter the profession describe it as a calling one that carries spiritual weight and a sense of sacred responsibility toward those who suffer. When systemic barriers prevent nurses from fulfilling that responsibility the resulting moral distress can be profound. The Tufts nurses concerns extend beyond physical working conditions to encompass this inner conflict. Professionals find themselves caught between their oath to advocate for patients and the practical limitations imposed by staffing decisions. This tension creates a form of injury to the spirit that no compensation package can fully remedy. Healthcare has always involved both technical skill and human compassion yet current conditions appear to be diminishing the latter in ways that may have long term consequences for the soul of the profession itself.
Potential Paths Toward Resolution

Finding solutions will require genuine collaboration between nurses administration and regulatory bodies. Mandatory staffing ratios specific to operating rooms could provide clearer guidelines though implementation details remain contentious. Enhanced retention bonuses tied to years of service might help stabilize the experienced workforce that currently feels most depleted. Investment in ongoing education programs could accelerate the development of new specialists while improved mental health resources would address the burnout that drives many departures. Some experts suggest partnerships with local nursing schools to create dedicated pipelines of talent familiar with Tufts specific needs. Whatever combination ultimately emerges success will depend on sustained commitment rather than temporary fixes. The nurses have indicated willingness to participate in good faith negotiations provided they see tangible movement toward safer conditions.
Looking to the Future of Healthcare Staffing

The outcome of this conflict at Tufts Medical Center may influence similar debates unfolding at other institutions nationwide. As demographic shifts bring an older population with greater surgical needs the pressure on operating room staff will only increase. Technological advances such as robotic assistance and remote monitoring offer some promise for reducing physical demands but cannot replace human judgment and presence. The coming years will test whether healthcare systems can realign their priorities to place adequate staffing at the center of operational planning. For middle aged readers who may one day find themselves or their loved ones on the operating table these Tufts nurses concerns represent more than a labor dispute. They reflect fundamental choices about what kind of care society values enough to properly fund and support.
Community Support and Public Awareness

Public response to the nurses position has been largely sympathetic with patient advocacy groups adding their voices to calls for reform. Community members recognize that safe surgical care depends on healthy working conditions for those who deliver it. Local leaders have urged both sides to reach agreement before the dispute affects access to scheduled procedures. Greater transparency about staffing levels and safety data could help rebuild trust between the hospital and the families it serves. As coverage of the situation spreads awareness grows about the hidden costs of understaffing that often remain invisible until a crisis emerges. The Tufts nurses concerns have sparked important conversations about the true meaning of healing environments and the people who sustain them through their daily dedication and expertise. Only through continued attention and informed dialogue can lasting improvements take root.