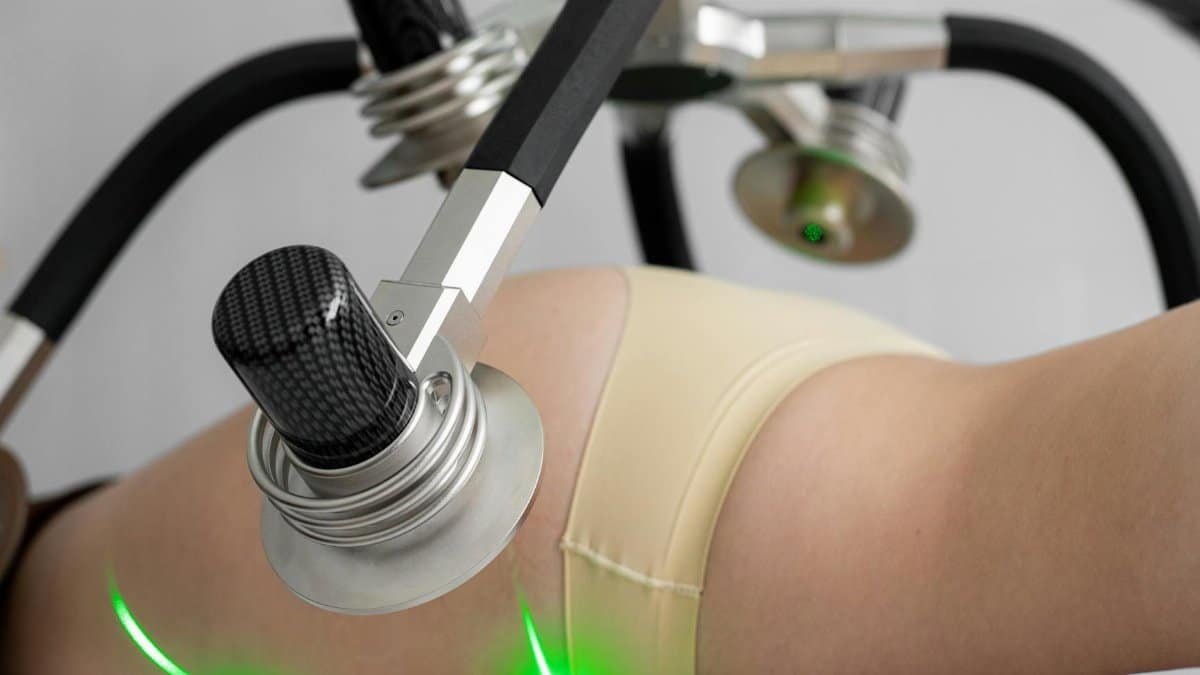
For many Americans navigating their middle years, persistent pain has become a silent thief of vitality. Backaches that linger after decades of desk work, joint inflammation that makes gardening difficult, arthritis that complicates simple tasks like opening jars. These struggles are familiar to millions, yet the standard medical response has too often led down a troubling path of heavy medications and their well documented consequences. In response, a meaningful shift is taking place inside clinics from coast to coast. Non-invasive pain management now stands at the center of this evolution, offering routes to relief that engage the body’s own systems rather than overriding them with drugs or scalpels.
Patients are discovering that pain need not define their remaining decades. By combining established medical insight with practices that address both physical sensation and mental experience, physicians are helping people reclaim daily life. The approach feels particularly resonant at this cultural moment when many seek gentler, more integrated ways to age with dignity and presence.
The Opioid Crisis Creates Space for New Solutions
The urgency behind this change traces directly to the opioid epidemic that has touched countless families. As overdose deaths mounted and addiction became a national crisis, medical leaders began searching for responsible alternatives. Hospitals and outpatient centers responded by expanding programs that prioritize methods without chemical dependency risks. What began as experimental offerings has moved steadily into standard protocols, especially for older adults who face higher dangers from long-term medication use.
Clinics now routinely screen patients for suitability for these approaches before considering stronger prescriptions. The results have been encouraging. Many individuals who once felt trapped by their pain report regaining function without the fog or withdrawal that can accompany opioid therapy. This transformation reflects both medical necessity and a deeper cultural reevaluation of how healing should occur.
Mindfulness Enters Mainstream Medical Settings

One of the most significant developments involves structured mindfulness training. No longer confined to spiritual retreats, these practices have been adapted into eight-week clinical programs with measurable outcomes. Participants learn to observe pain sensations without immediate panic or resistance, often experiencing a surprising decrease in perceived intensity.
Neurological imaging reveals why this works. Regular mindfulness appears to quiet activity in brain regions associated with pain amplification while strengthening areas tied to emotional regulation. For middle-aged patients balancing careers, family responsibilities and their own aging bodies, this mental training offers practical relief that extends beyond the treatment room. Many describe feeling more equipped to handle life’s stresses even as their physical discomfort diminishes.
Acupuncture Finds Validation in American Clinics
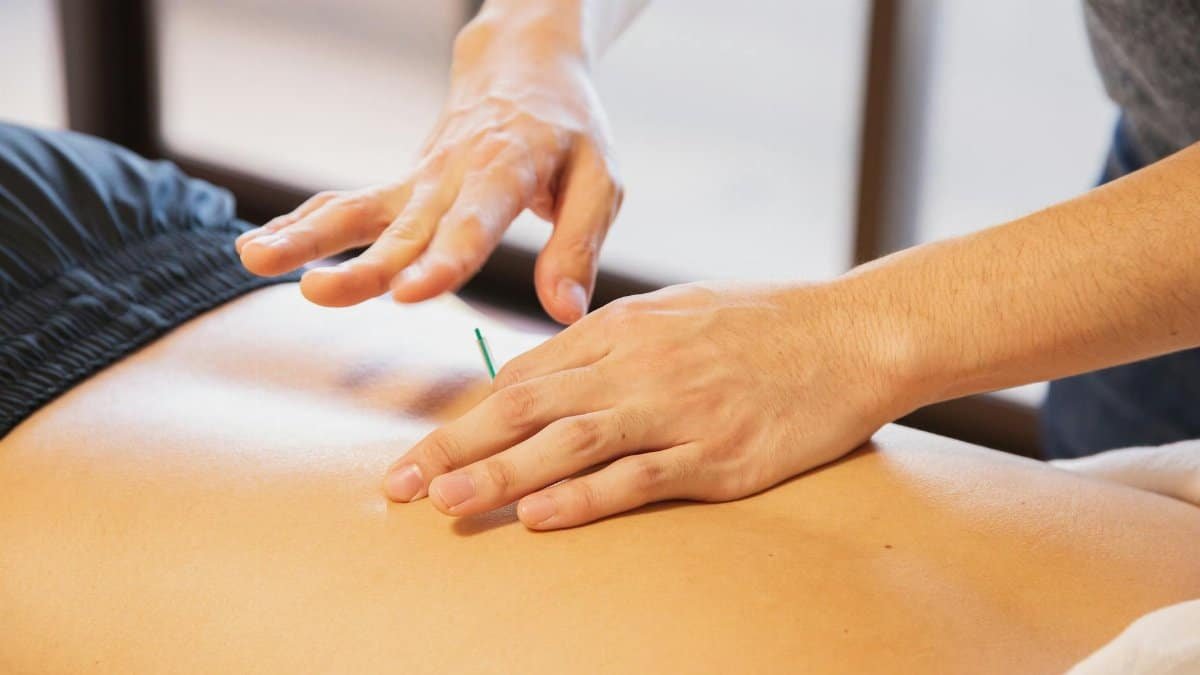
Acupuncture has traveled a long path from skepticism to acceptance. Major health systems in cities like Los Angeles and Philadelphia now employ licensed practitioners alongside conventional doctors. The technique involves strategic placement of fine needles that stimulate nerve pathways and encourage natural pain-relieving chemicals within the body.
Large scale reviews of clinical data support its use for conditions including migraines, osteoarthritis and chronic back problems. Patients often appreciate that sessions create space for quiet reflection, an element that aligns with many people’s desire for care that acknowledges their full humanity rather than treating them as collections of symptoms. Insurance coverage has expanded in many states, removing a once formidable barrier to access.
Biofeedback Technology Bridges Mind and Body

Modern biofeedback represents another frontier. Using sensors that monitor muscle tension, heart rate variability and skin temperature, patients learn to influence bodily processes once considered automatic. The technology provides real-time data that makes invisible shifts visible, empowering individuals to participate actively in their own relief.
Clinics report particular success with older adults who enjoy the concrete feedback and sense of mastery it provides. Rather than feeling helpless before their pain, they develop tangible skills that travel with them beyond the appointment. Some programs combine biofeedback with breathing techniques drawn from contemplative traditions, creating an experience that feels both technological and deeply personal.
Virtual Reality Opens New Pathways for Relief

Virtual reality has moved from gaming worlds into medical suites with surprising effectiveness. Patients don headsets that transport them to serene landscapes or engaging scenarios designed specifically for pain reduction. The immersive distraction appears to interrupt pain signaling while also reducing associated anxiety.
Research facilities in Texas and New York are documenting how customized virtual environments can help patients undergoing uncomfortable procedures or dealing with chronic symptoms. For middle-aged adults who grew up before widespread digital technology, the experience can feel like science fiction in service of healing. Many report that the mental respite lasts well after the headset comes off.
Movement Practices with Ancient Roots

Yoga and tai chi have gained substantial traction as therapeutic tools. Adapted classes in clinical settings focus on gentle movement, breath awareness and balance rather than athletic performance. These practices seem particularly valuable for adults concerned about bone density, flexibility and fall risk as they age.
Physical therapists increasingly incorporate elements of these disciplines, recognizing that mindful movement creates benefits beyond simple exercise. Participants often speak of improved sleep, better mood and a renewed connection to their bodies. The spiritual dimensions many find in these practices, even when presented in secular medical contexts, appear to enhance their healing potential for those so inclined.
Music and Sound Therapy Gain Clinical Respect

Another development involves therapeutic use of sound. From carefully selected musical playlists to devices that emit specific frequencies, clinics are exploring how auditory experiences can modulate pain perception. Some programs use live musicians who adapt in real time to patients’ responses.
This approach carries special appeal for those who may struggle with traditional talk-based therapies. The non-verbal nature of music creates an accessible entry point, particularly for men who grew up in generations less comfortable discussing emotional aspects of health. Emerging evidence suggests these interventions can reduce reliance on medication while improving emotional resilience.
Real Patient Stories from Across America

The human dimension of these changes becomes clear through individual experiences. Margaret Chen, a 62-year-old retired teacher from Oregon, had lived with severe sciatica for seven years before trying a comprehensive non-invasive pain management program. After three months combining mindfulness, acupuncture and movement therapy, she resumed volunteer work at her local library and began hiking again on easier trails.
Similar accounts emerge from Minnesota to Florida. A construction worker in his late 50s learned biofeedback techniques that allowed him to reduce his pain medication by more than half. A woman managing both fibromyalgia and anxiety found that virtual reality sessions helped break the fear-pain cycle that had dominated her life. These stories illustrate how non-invasive pain management addresses the whole person rather than isolated symptoms.
What Current Research Actually Shows

Scientific validation has been crucial to this shift. A major analysis published by the National Institutes of Health examined more than 200 studies and found moderate to strong evidence for several non-invasive approaches, particularly for chronic lower back pain and osteoarthritis. Results for mindfulness interventions appear especially promising when programs follow established protocols.
Longer-term studies are still needed, yet early findings suggest these methods may help prevent the brain changes associated with chronic pain states. This possibility excites researchers because it points toward actual healing rather than symptom management. Medical journals that once dismissed such approaches now regularly feature rigorous trials, signaling a genuine evolution in evidence-based medicine.
Obstacles to More Widespread Use

Despite encouraging developments, significant challenges remain. Insurance reimbursement varies widely by state and provider. Many patients still encounter skepticism from practitioners trained in more traditional models. Access can be especially difficult in rural areas where specialized clinics remain rare.
Training sufficient numbers of qualified practitioners represents another hurdle. While interest grows, the pathway to certification in integrative approaches requires time and resources. Additionally, some patients arrive with unrealistic expectations after encountering overstated claims online. Managing these expectations while maintaining hope requires skilled communication from care teams.
Toward More Integrated Healing Models

The most forward-looking clinics are building teams that combine conventional physicians, physical therapists, mindfulness instructors and movement specialists. This collaborative model acknowledges that pain exists at the intersection of biology, psychology, social connection and, for many, spiritual experience. Rather than forcing patients to choose between mainstream and alternative care, these centers create coherent treatment plans tailored to individual needs and values.
As the population ages, the demand for such thoughtful approaches will only increase. The goal extends beyond reducing pain numbers on a chart. It involves helping people remain engaged with work, family, community and their own sense of purpose even as bodies change. Non-invasive pain management, when practiced with skill and compassion, offers a path toward that fuller participation in life.
The quiet revolution happening in examination rooms and therapy spaces across the country suggests a more humane vision of medical care, one that honors both scientific rigor and the complex realities of human suffering. For millions of middle-aged Americans, these advances arrive not a moment too soon.